Still looking for that gift that does not involve screen time? We’re reposting our back-to-basics gift ideas post:
0-3 months: Babies this age have perfect hearing and enjoy looking at faces and objects with contrasting colors. Music, mobiles, and bright posters are some age appropriate gift ideas. Infants self-soothe themselves through sucking- if you can figure out what your nephew’s favorite type of binkie is, wrap up a bunch-they are expensive and often mysteriously disappear.
3-6 months: Babies start to reach and grab at objects. They enjoy things big enough to hold onto and safe enough to put in their mouths- try bright colored teething rings and large plastic “keys.” We often see Sophie the Giraffe accompanying babies for their office visits. New cloth and vinyl books will likewise be appreciated; gnawed books don’t make great hand-me-downs.
6-12 months: Around six months, babies begin to sit up. Intellectually, they begin to understand “cause and effect.” Good choices of gifts include toys with large buttons that make things happen with light pressure. Toys which make sounds, play music, or cause Elmo to pop up will be a hit. For a nine-month-old old just starting to pull herself up to a standing position, a water or sand table will provide hours of entertainment in the upcoming year. Right now you can bring winter inside if you fill the water table with a mound of snow. Buy some inexpensive measuring cups and later in the summer a toddler will enjoy standing outside splashing in the water.
12-18 months: This is the age kids learn to stand and walk. They enjoy things they can push while walking such as shopping carts or plastic lawn mowers. Include gifts which promote joint attention. Joint attention is the kind of attention a child shares with people during moments of mutual discovery. Joint attention starts at two months of age when a parent smiles at their baby and their baby smiles back. Later, around 18 months, if a parent points at a dog in a book, she will look at the dog then look back at the parent and smile. A child not only shows interest in the same object, but will acknowledge that both she and the parent are interested. Joint attention is thought to be important for social and emotional growth.
18-24 months: Although kids this age cannot pedal yet, they enjoy riding on toys such as “big wheels” “Fred Flintstone” style. Dexterous enough to drink out of a cup and use a spoon and fork, toddlers can always use another place setting. Toddlers are also able to manipulate shape sorters and toys where they put a plastic ball into the top and the ball goes down a short maze/slide. They also love containers to collect things, dump out, then collect again.
Yes, older toddlers are also dexterous enough to swipe an ipad, but be aware, electronics can be a double edged sword— the same device which plays karaoke music for your daddy-toddler sing-along can be transformed into a substitute parent. The other day, a toddler was frightened of my stethoscope in the office. Instead of smiling and demonstrating to her toddler how a stethoscope does not hurt, the mother repeatedly tried to give her toddler her phone and told the child to watch a video. Fast forward a few years, and the mother will wonder why her kid fixates on her phone and does not look up at the family at the dinner table. Don’t train an addiction. A device can be entertainment, learning, and communication but it is NOT a source of comfort.
2-3 years: To encourage motor skills, offer tricycles, balls, bubbles, and boxes to crawl into and out of. Choose crayons over markers because crayons require a child to exert pressure and therefore develop hand strength. Dolls, cars, and sand boxes all foster imagination. Don’t forget those indestructible board books so kids can “read” to themselves. By now, the plastic squirting fish bath toys you bought your nephew when he was one are probably squirting out black specks of mold instead of water- get him a new set. Looking ahead, in the spring a three- year-old may start participating in team sports (although they often go the wrong way down the field) or in other classes such as dance or swimming lessons. Give your relatives the gift of a shin guards and soccer ball with a shirt. Offer to pay for swim lessons and package a gift certificate with a pair of goggles.
3-4 years: Now kids engage in elaborate imaginary play. They enjoy “dress up” clothes to create characters- super heroes, dancers, wizards, princesses, kings, queens, animals. Kids also enjoy props for their pretend play, such as plastic kitchen gadgets, magic wands, and building blocks. They become adept at pedaling tricycles or even riding small training-wheeled bikes. Other gift ideas include crayons, paint, markers, Play-doh®, or side-walk chalk. Children this age understand rules and turn-taking and can be taught simple card games such as “go fish,” “war,” and “matching.” Three-year-olds recognize colors but can’t read- so they can finally play the classic board game Candyland, and they can rote count in order to play the sequential numbers game Chutes and Ladders. Preschool kids now understand and execute the process of washing their hands independently… one problem… they can’t reach the faucets on the sink. A personalized, sturdy step stool will be appreciated for years.
5-year-olds: Since 5-year-olds can hop on one foot, games like Twister® will be fun. Kids this age start to understand time. In our world of digital clocks, get your nephew an analog clock with numbers and a minute hand… they are hard to come by. Five-year-olds also begin to understand charts— a calendar will also cause delight. They can also work jigsaw puzzles with somewhat large pieces.
8-year-olds: Kids at this point should be able to perform self help skills such as teeth brushing. Help them out with stocking stuffers such as toothbrushes with timers. They also start to understand the value of money so kids will appreciate gifts such as a real wallet or piggy bank. Eight-year-olds engage in rough and tumble play and can play outdoor games with rules. Think balls, balls, balls- soccer balls, kickballs, baseballs, tennis balls, footballs. Basic sports equipment of any sort will be a hit. Label makers will also appeal to this age group since they start to have a greater sense of ownership.
10-year-olds: Fine motor skills are quite developed and intricate arts and crafts such as weaving kits can be manipulated. Give a “cake making set” (no, not the plastic oven with a light bulb) with tubes of frosting and cake mix to bake over the winter break. Kids at this age love doodling on the long rolls of paper on our exam table. Get a kid a few rolls of banner paper to duplicate the fun. Buy two plastic recorders, one for an adult and one for a child, to play duets. The instrument is simple enough for ten-year-olds or forty-year-olds to learn on their own. Ten-year-olds value organization in their world and want to be more independent. Therefore, a watch makes a good gift at this age. And don’t forget about books: reading skills are more advanced at this age. They can read chapter books or books about subjects of interest to them. In particular, kids at this age love a good joke or riddle book.
Tweens: Your child now has a longer attention span (30-40 minutes) so building projects such as K’nex models will be of interest to her. She can now also understand directions for performing magic tricks or making animal balloons. This is a time when group identity becomes more important. Sleepovers and scouting trips are common at this age so sleeping bags and camping tents make great gifts. Tweens value their privacy – consider a present of a journal with a lock or a doorbell for her room. It’s already time to think about summer camps. Maybe you can convince the grandparents to purchase a week for your child at robotics camp or gymnastics camp this year.
Teens: If you look at factors which build a teen into a resilient adult, you will see that adult involvement in a child’s life is important. We know parents who jokingly say they renamed their teens “Door 1” and “Door 2,” since they spend more time talking to their kids’ bedroom doors than their kids. Create opportunities for one-on-one interaction by giving gifts such as a day of shopping with her aunt, tickets to a show with her uncle, or two hours at the rock climbing gym with dad.
Encourage physical activity. Sports equipment is always pricey for a teen to purchase- give the fancy sports bag he’s been eying or give a gym membership. Cool techy trackers like Fitbit will always appreciated or treat your teen to moisture wicking work-out clothes.
Sleep! Who doesn’t need it, and teens often short change themselves on sleep and fall into poor sleep habits. Help a teen enjoy a comfortable night of rest and buy luxurious high thread count pillow cases, foam memory pillows, or even a new mattress. After all, it been nearly 20 years since you bought your teen a mattress and he probably wasn’t old enough at the time to tell you if he was comfortable. Since a teen often goes to bed later than you do, a remote light control will be appreciated by all.
Adolescence is the age of abstract thinking and self awareness— Google “wall decals” and find a plethora of inexpensive ways to jazz up his or her room with inspiring quotes.
Enjoy your holiday shopping.
Naline Lai, MD and Julie Kardos, MD
©2018 Two Peds in a Pod®



 You don’t appreciate how much your baby has grown until you attempt a diaper change on a plane. For families, any holiday can become stressful when traveling with young children is involved. Often families travel great distances to be together and attend parties that run later than their children’s usual bedtimes. Fancy food and fancy dress are common. Well-meaning relatives who see your children once a year can be too quick to hug and kiss, sending even not-so-shy kids running. Here are some tips for safer and smoother holiday travel:
You don’t appreciate how much your baby has grown until you attempt a diaper change on a plane. For families, any holiday can become stressful when traveling with young children is involved. Often families travel great distances to be together and attend parties that run later than their children’s usual bedtimes. Fancy food and fancy dress are common. Well-meaning relatives who see your children once a year can be too quick to hug and kiss, sending even not-so-shy kids running. Here are some tips for safer and smoother holiday travel:
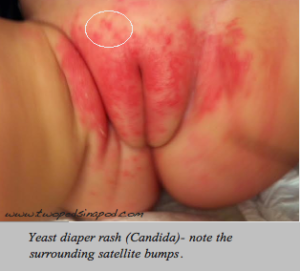 Yeast rash
Yeast rash