Stealthy Salmonella! Not just in your eggs
Raw chicken left out overnight—Dr. Lai’s recipe for Salmonella
These days it seems that the bacteria Salmonella is lurking everywhere. Last month’s egg recall for possible Salmonella contamination affected over 200 million eggs, but Salmonella is not just in eggs. In the last few months, dried coconuts and even guinea pigs (as pets, not as food!) have caused people gastroentestinal misery.
Nontyphoidal Salmonella usually causes fever and crampy diarrhea. Sometimes the stools contain blood. This stomach bug mainly lurks in raw poultry, raw eggs, raw beef, and unpasturized dairy products. Luckily, Salmonella does not jump up and attack humans. In general, people are safe from disease as long as they do not eat salmonella-infested food. But children below the age of five often put their hands in their mouths and can acquire Salmonella after touching a contaminated source.
Reptiles such as lizards and turtles can carry Salmonella in their stool and are not recommended as pets for young children. Turtles that are four inches or smaller (about the size of a deck of playing cards) are most likely to harbor the bacteria. As a preschooler, Dr. Kardos remembers that her tiny pet turtle suddenly disappeared. Her parents told her that “Her pet would be happier if it went outside to the stream to swim with the other turtles.” In retrospect, Dr. Kardos thinks her pediatrician dad was worried about Salmonella and made the turtle magically disappear.
Even cute little chicks can be problematic. Salmonella carried in the gut of a chick can contaminate the entire surface of a chick. So, although kissing and cuddling a chick makes for a good Instagram post, discourage your children from doing so.
Unfortunately, you cannot depend on a warning stench arising from your lunch to warn you that it is inedible. Salmonella often hides in food and it is difficult to tell what is or is not contaminated. So how can you prevent your kids from catching Salmonella?
Luckily Salmonella is killed by heat and bleach. Even if an otherwise fine-looking and odorless raw egg has Salmonella, adequate cooking will destroy the bacteria. Gone are the days when parents can feed kids soft boiled eggs in a silver cup, have kids wipe up with toast the yolk from a sunny-side up egg, add a raw egg to a milkshake, or let their kids lick the left-over cake batter from the mixing bowl. Instead, cook hardboiled eggs until the yolks are green and crumble, and make sure your scrambled eggs aren’t runny. Wash all utensils well. The disinfecting solution used in childcare centers of ¼ cup bleach to 1 gallon water works well to sanitize counters. Do not keep perishable food, even if it is cooked, out at room temperature for more than two hours. And wash, wash, wash your hands.
A mom once called us frantic because her child had just happily eaten a half-cooked chicken nugget. What if this happens to your child? Don’t panic. Watch for symptoms — the onset of diarrhea from Salmonella is usually between 12 to 36 hours after exposure but can occur up to three days later. The diarrhea can last up to 5-7 days. If symptoms occur, the general recommendation is to ride it out. Prevent dehydration by giving plenty of fluids. My simple rule to prevent dehydration is that more must go in than comes out.
Although of unproven benefit, antibiotic treatment may be considered if your child is at risk for overwhelming infection, including infants younger than three months old and those with abnormal immune systems (cancer, HIV, Sickle Cell disease, kids taking daily steroids for other illnesses) or those with chronic gastrointestinal tract diseases*. Using antibiotics to treat a typical case of salmonella not only promotes general antibiotic resistance, but also does not shorten the time frame for the illness. In fact, the medication can prolong how long your child carries the germ in his stool.
Pictured above is a pot of chicken Dr. Lai accidentally left out overnight one warm summer night. Yuck.
Naline Lai, MD and Julie Kardos, MD
©2018 Two Peds in a Pod®
*Red Book, 2015 Report of the Committee on Infectious Diseases, American Academy of Pediatrics


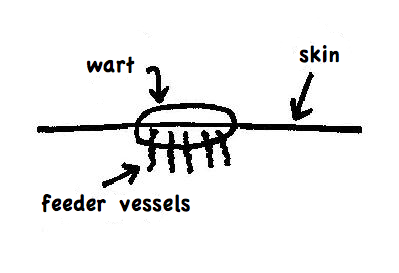
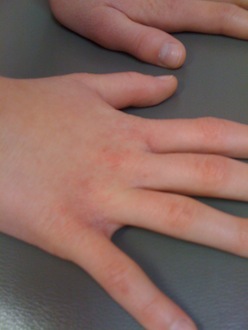
 It’s time for another Two Peds in a Pod photo quiz.
It’s time for another Two Peds in a Pod photo quiz.




 In light of the recent school shooting in Parkland, Florida, you may be left wondering if, and how, to explain this or other tragedies to your children.
In light of the recent school shooting in Parkland, Florida, you may be left wondering if, and how, to explain this or other tragedies to your children.